Here we go again...
We Burwicks enjoy a good roller coaster as much as anyone else from time to time....just not the emotional kind. Not to be overdramatic – but we're not in Disney World anymore! In fact, it feels like we've been on a bit of an emotional roller coaster for the past couple of weeks.
BUCKLE IN...
On February 20, Bryan returned to Mayo Clinic for a regular CT scan as part of his continued post-surgery follow-up. We were praying that we would see the 3 tiny spots on his left lung disappear, even though he hasn't been undergoing treatment since early July. We knew they were still there as of the time of his CT scan back in November, but way too small to biopsy or anything, so we weren't sure whether they were cancerous or something else.
GOING UP...
Bryan met with his oncologist at Mayo on February 24 for the radiology results, and she had good news and not-so-great news to share with him. She said the CT scans and bloodwork showed that the surgical sites (colon, liver, right lung) were clear of cancer and functioning well. All glory to God!
...and DROP!
However, the 3 tiny spots on his left lung had changed slightly over the past few months. One had shrunk from 6mm to 5mm, while the other two had increased 2mm each – from 6mm to 8mm, and 8mm to 10mm. Based on this finding, she had already consulted with his lung surgeon, and they determined that the spots were acting more like cancer than not. So, they recommended that it's time to begin a 12-16 week round of chemotherapy once again, to stay ahead of any more growth or spreading of cancer in his body.
Bryan & I were pretty disappointed and discouraged on the day we got this news, and we allowed ourselves to take the day to grieve and be sad that we are having to deal with chemo once again. It felt a little bit like PTSD from our past experience with cancer & chemo. But we also know that the SAME God who has brought miraculous healing to him before is STILL with us today. And the same family & friends who have prayed and supported us since his initial diagnosis in 2024 are still praying and supporting us now. We have HOPE that the chemo will be effective, as it was before, and that Bryan will tolerate it as well as he did last time too. He is no longer anemic, feels much stronger and more energetic, and has much less cancer in his body than he did at the beginning of his first round of chemo, so he is at a much better starting point this time. Praise the Lord!
TURN #1
Another interesting thing the CT scan showed was the tube from his chest port, which is supposed to drop into a major artery that flows directly into his heart (Superior Vena Cava), was not in the correct position. Instead, it was pointing to a smaller vein that flows toward his spinal cord. This made it difficult to draw blood from the port, due to less blood flow from the smaller vein, and it's not the correct place to deposit medications. (Putting drugs into the heart ensures that it gets distributed immediately to the whole body.) This tube displacement isn't super common, but it can happen just from the patient coughing or sneezing hard, or doing significant physical activity. Bryan had been sick (coughing & sneezing) over the holidays, so maybe it happened then. At any rate, they tried a few different non-invasive ways to reposition the tube, but were unsuccessful. So, the only alternative was to replace the port & tube surgically. They scheduled the outpatient procedure right away, and got it done on Tuesday, March 3.
CLIMBING AGAIN...
With that out of the way, Bryan went ahead and scheduled his first treatment for Friday, March 6. The oncologist had noted that Bryan had suffered from neuropathy in his hands & feet during/since his previous chemotherapy, which is commonly known as FOLFOX/5-FU. Because she does not want his neuropathy to worsen with more chemo, she opted to change one of the drugs (oxaliplatin) to another one (irinotecan). So this chemotherapy is referred to as FOLFIRI/5-FU. There are other adverse side effects with this one, of course – so we're trading cold sensitivity & neuropathy for potential nausea, diarrhea, and hair loss. In fact, the nurses have jokingly given irinotecan a nickname of: "I run to the can." It might be funny if it weren't true.
Anyway...FOLFIRI follows the same 2-week infusion cycle (with a 2-day 5-FU pump) as the previous treatment. At our previous cancer center, we would have to physically go in 4 times during each treatment week: blood draw/labs on Saturday, doctor appointment on Monday, infusion treatment on Wednesday, and pump disconnection on Friday. At Mayo, they will do the first three things all in ONE DAY! Blood draw, doctor appointment, and infusion. Then, they are going to train & certify me (Kelley) to remove the pump AT HOME after 2 days, so we only have to make the trip to Mayo one day out of every 2 weeks. Thank you, Lord!
TURN #2
So, on Friday, March 6, we checked in for his blood draw appointment at 10:45am, and then waited for the oncologist to review the results and approve the treatment. (We took the selfie below while we were in the beautiful waiting room with a massive picture window overlooking the surrounding desert & mountains from the third floor.)
At 12:30pm, they called us back to the infusion center, where Nurse Kyla (How comforting that she shares the same name as our niece, who is also in the medical field!) greeted us and showed us where we would be hanging out for the next few hours. Nurse Kyla had four cubicles facing each other where she could monitor & administer treatments to the patients for whom she was caring. Our cubicle faced another window, so we had a wonderful view again.
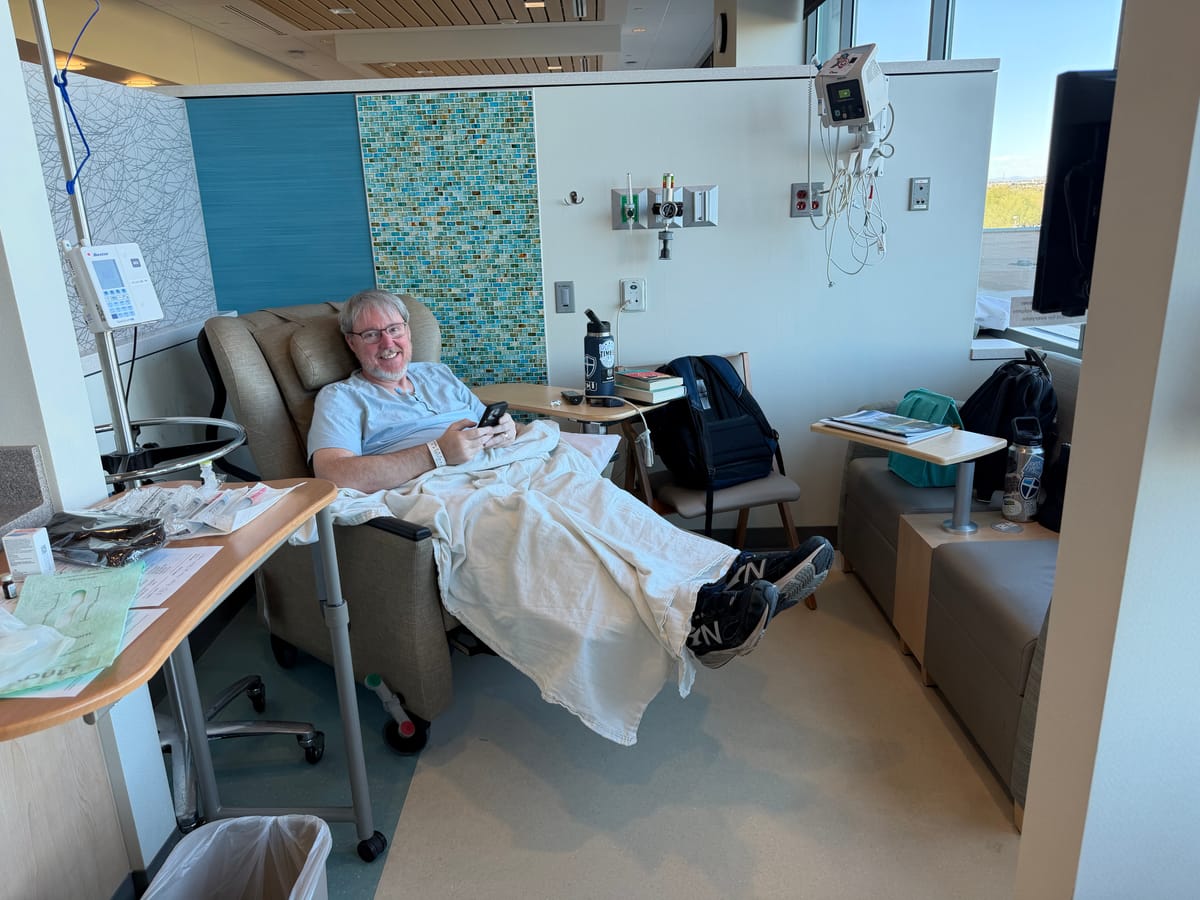
The photo at the top of this post shows Bryan smiling because for the first time on this chemo journey, I was allowed to sit with him the whole time. For context, you must understand...at our previous treatment center, there was just one infusion room with several rows of chairs for patients, but only a couple nurses on duty and NO guests allowed. I would literally have to drop him off and leave him there for several hours until his infusion was finished, and then come back and pick him up. It was heartbreaking! Here, the infusion center takes up half of the whole floor, and we can bring in our laptops, books, card games, snacks, etc. to pass the time together.
LoOp-de-lOoP!
There was one little hiccup with this first treatment, in that Bryan had forgotten to take his blood pressure medicine before we left the house, and his readings were too high. Nurse Kyla patiently took his blood pressure three times, giving him several minutes to rest between. But, it remained stubbornly elevated, so she called his oncologist and they decided to go ahead with treatment, but leave out one immunotherapy drug (avastin), which is supposed to amplify the effectiveness of the other chemo drugs, but it raises the patient's blood pressure in the process.
RETURNING TO THE STATION
Nurse Kyla began the treatment by first administering anti-nausea & anti-diarrhea medications, and then the chemo drug (irinotecan). She warned that Bryan might experience the effects of the new drug – cramping and urgency in his bowels – even as soon as during the treatment. Fortunately, he had been fasting the day prior and day of treatment (based on some research he had done about minimizing side effects), so he felt fine during the treatment and our 45-minute commute home. After we got home, I made him some food and he spent the evening watching TV with me on the couch.
Since the first treatment on Friday, he has felt fairly normal. He hasn't experienced any extreme side effects yet, but we are aware that chemo may have a worsening cumulative effect with more treatments over the next few months. His stomach has felt upset when he first awakens in the morning, but once he eats something, he feels better. So far, his digestion seems to be functioning pretty normally as well. Today (Sunday), Bryan has felt very sleepy – dozing on the couch off and on for most of the day.
WHAT A RIDE!
For now, we are grateful to God for each day, learning to recognize how much we've been through in the past 18 months – and be kind to ourselves and each other. We are currently re-learning the roller coaster of how to deal with the unfortunately familiar circumstances in which we find ourselves, and also remembering how to open our eyes to see and open our hearts to love those whom the Lord places in our path each day.
Continued prayers appreciated!
"And do not be grieved, for the joy of the Lord is your strength." ~ Nehemiah 8:10
"My flesh and my heart may fail, but God is the strength of my heart and my portion forever." ~ Psalm 73:26
